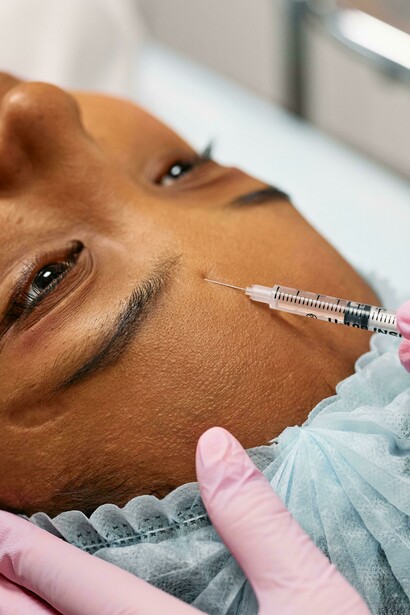
Aesthetic medicine has evolved far beyond the treatment of facial wrinkles. Over the last decade, the specialty has expanded into areas once rarely discussed in clinical practice or public conversation: the aesthetics and functional health of intimate anatomy. Among the newest and most debated procedures within this emerging field is the use of botulinum toxin injections in the penis — a treatment sometimes informally referred to as “Bocox.”
While the name may sound surprising, the scientific rationale behind the procedure is grounded in mechanisms physicians understand well. Botulinum toxin, widely known for its use in facial rejuvenation, works by temporarily blocking nerve signals that trigger muscle contraction. When muscles relax, tissues behave differently: tension decreases, circulation may improve, and the physical appearance of the area can change.
These same physiological principles are now being explored in male sexual medicine. Researchers and clinicians are investigating whether botulinum toxin injections into penile tissue may improve certain forms of erectile dysfunction and influence how the penis behaves in its flaccid state. Although the concept remains relatively new, it reflects a broader transformation in the way medicine approaches male health, sexual wellness, and aesthetic confidence.
Understanding the physiology behind penile Botox
To appreciate why botulinum toxin might play a role in male sexual health, it is important to consider the basic physiology of erections. Erectile function depends on a complex interaction between nerves, blood vessels, hormones, and smooth muscle tissue within the penis. During sexual stimulation, smooth muscle fibers in the corpora cavernosa — the erectile bodies — relax, allowing blood to fill the spaces within the tissue and produce rigidity.
Botulinum toxin works by inhibiting the release of acetylcholine at neuromuscular junctions. This temporarily interrupts the communication between nerves and muscles, leading to muscle relaxation. In theory, when injected into penile tissue, the toxin may help reduce excessive smooth muscle contraction, potentially facilitating improved blood flow within the erectile bodies.
For certain patients — particularly those who do not respond adequately to conventional medications such as phosphodiesterase-5 inhibitors — this mechanism could offer a complementary therapeutic strategy. Early clinical studies suggest that intracavernosal injections of botulinum toxin may enhance erectile function in selected cases by promoting a more relaxed vascular environment within the penis.
From a procedural perspective, the treatment is relatively straightforward. Using a very fine needle, a trained physician administers small doses of botulinum toxin into targeted areas of the penile tissue. The procedure typically takes only a few minutes and is performed in an outpatient setting. Most patients experience minimal discomfort, and daily activities can usually be resumed shortly afterward.
The effects of the toxin develop gradually over several days and typically persist for several months before the body naturally metabolizes the compound.
Aesthetic implications and the “flaccid appearance”
Beyond its potential therapeutic role in erectile dysfunction, penile Botox has also attracted interest for its aesthetic effects. One of the most frequently discussed outcomes is a change in the appearance of the penis in its non-erect state.
The penis contains smooth muscle fibers that can contract in response to factors such as cold temperature, stress, or physical activity. This contraction can cause the penis to retract toward the body — a physiological reaction often described colloquially as “shrinkage.”
By relaxing these muscles, botulinum toxin may reduce the tendency for this retraction to occur. As a result, the penis may appear somewhat fuller or longer in its flaccid state. It is important to emphasize that the treatment does not increase anatomical size. Rather, it alters the resting behavior of the tissues, which can influence visual perception.
In aesthetic medicine, perception often plays an important role in patient satisfaction. For some individuals, this subtle change in appearance may improve self-confidence or body image, particularly in environments such as sports or communal changing rooms where flaccid appearance becomes a psychological concern.
The rise of male intimate aesthetic medicine
The growing interest in procedures such as penile Botox reflects a larger shift occurring within aesthetic medicine: the rapid increase in male patients seeking treatments that address both appearance and functional wellness.
Historically, cosmetic procedures were largely marketed toward women. However, recent years have seen a dramatic expansion in male participation in aesthetic clinics. Treatments such as neuromodulators, dermal fillers, and laser therapies are now commonly requested by men seeking subtle enhancements without surgery.
Intimate aesthetic procedures represent the next stage in this evolution. As cultural attitudes toward male self-care continue to change, discussions about sexual health, body image, and confidence are becoming more open. Patients increasingly approach physicians not only for medical treatment but also for guidance in optimizing their sense of wellbeing.
In this context, penile Botox exists at the intersection of aesthetic dermatology, urology, and sexual medicine.
A brief note on scrotal Botox
Another procedure that occasionally appears in the same conversation is scrotal botulinum toxin injections, popularly referred to as “Scrotox.” While less studied from a medical standpoint, the treatment is typically sought for aesthetic and comfort-related reasons rather than erectile function.
Botulinum toxin injected into the scrotal skin can relax the dartos muscle, which is responsible for tightening and wrinkling the scrotum in response to temperature changes. Relaxation of this muscle may produce a smoother and slightly more relaxed appearance of the scrotal skin. Some patients also report reduced sweating or improved comfort in hot climates.
Although scrotal Botox is often discussed alongside penile injections, the therapeutic objectives are quite different. Penile Botox is primarily being investigated for its potential role in erectile physiology, whereas scrotal Botox is largely aesthetic.
Scientific evidence and ongoing research
While the media attention surrounding Bocox might suggest a sudden breakthrough, the scientific exploration of botulinum toxin in erectile dysfunction has been developing quietly for several years.
Clinical studies have examined the use of intracavernosal botulinum toxin injections as an adjunct therapy for men who do not respond adequately to standard pharmacological treatments. Early results have shown encouraging improvements in erectile function scores in certain patient populations.
However, it is important to acknowledge that the field remains in its early stages. Large-scale randomized trials are still limited, and standardized protocols for dosage and injection technique have yet to be universally established. As with many innovative therapies, the enthusiasm surrounding the procedure must be balanced with rigorous scientific evaluation.
Responsible physicians must therefore approach the technique with both curiosity and caution, ensuring that patient safety and ethical medical practice remain the primary priorities.
Managing expectations and maintaining medical responsibility
As with any emerging aesthetic or medical trend, managing patient expectations is essential. Penile Botox is not a universal solution for erectile dysfunction, nor is it a method of permanent penile enlargement. Its potential benefits appear most relevant in carefully selected patients and within the context of a comprehensive medical evaluation.
Possible side effects are generally mild and may include temporary swelling, bruising, or discomfort at the injection site. Because botulinum toxin is temporary, its effects gradually diminish over several months, meaning maintenance treatments would be required for sustained results.
More importantly, erectile dysfunction can sometimes be a sign of broader health issues, including cardiovascular disease, metabolic disorders, or hormonal imbalance. For this reason, physicians must ensure that aesthetic interest does not overshadow the importance of proper medical diagnosis.
In many cases, the most effective treatment approach may involve a combination of lifestyle changes, pharmacological therapy, psychological support, and, in selected situations, innovative procedures such as botulinum toxin injections.
A reflection of changing conversations around men’s health
The emergence of penile Botox ultimately tells a larger story about how medicine and society are evolving. For decades, male sexual concerns were often hidden behind stigma or embarrassment. Today, patients are more willing to discuss these topics openly and seek professional guidance.
At the same time, physicians must navigate the influence of social media and public curiosity surrounding new procedures. Medical innovation can generate excitement, but it also requires careful communication to ensure that patients understand both the possibilities and the limitations of emerging treatments.
Penile Botox may or may not become a widely adopted therapeutic tool in the future. What is certain, however, is that it reflects a growing recognition that sexual health, aesthetic confidence, and overall well-being are deeply interconnected aspects of human life.
As aesthetic medicine continues to evolve, the responsibility of physicians is not simply to follow trends but to guide them with scientific rigor, ethical responsibility, and respect for patient well-being.
Author’s note
As a physician working in dermatology and aesthetic medicine, I believe the expansion of treatments into intimate areas must always be approached with responsibility and scientific caution. While procedures such as penile botulinum toxin injections show promising potential in selected patients, they should remain grounded in proper medical evaluation, ethical practice, and ongoing clinical research.