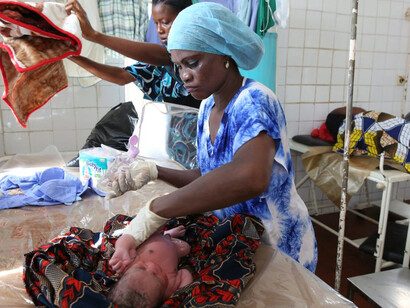
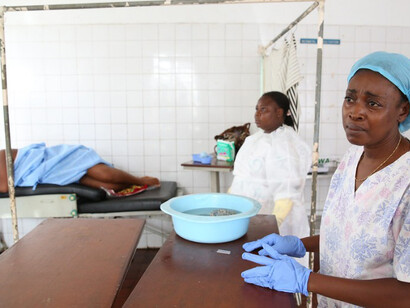
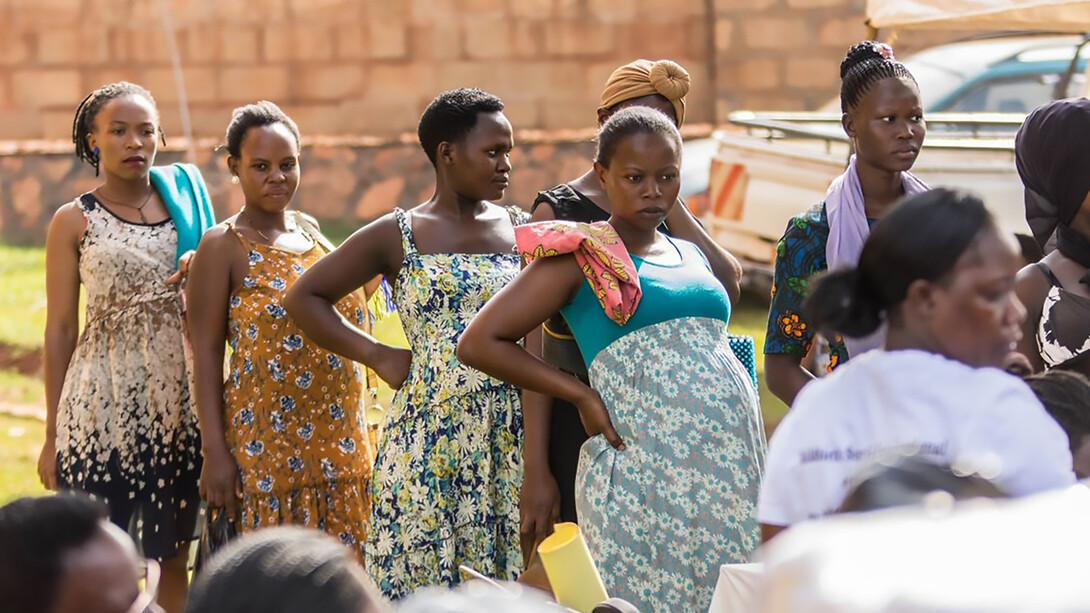Between 2000 and 2023, UNICEF reported a 40% decline in maternal mortality rates. However, there are still approximately 197 deaths per 100,000 live births. These maternal deaths are commonly observed among women of low-middle and low socioeconomic backgrounds.
These statistics remain as a reminder of whether innovations and progress in the healthcare system are actually working for women. Maternal deaths are preventable. Solutions for this lie in big data. To know what they might be, we need to understand what big data is and what its impact can really mean for maternal mortality rates.
What are current maternal mortality rates telling us?
While the global maternal mortality rates have declined, the past decade has seen stagnation in the efforts to further reduce these rates. 2023 alone saw 260,000 maternal deaths2. This means that one woman dies every two minutes from either pregnancy or delivery-related complications.
Between 2016 and 2020, WHO data showed3 that there was no improvement among 150 countries in improving the maternal mortality rates. This is currently jeopardizing the progress of SDG 3.1 to reduce maternal mortality to 70 per 100,000 women by 2030.
This slow progress places the heaviest burden on countries such as Africa and India and the lower socio-economic communities within other countries, such as Hispanics and Black women in North America. These demographic realities4 highlight the health inequalities, since there are advances in medical treatment, but they are not reaching everyone. This divide increases when disease outbreaks, public health emergencies, and other conflicts take precedence over a woman’s well-being during pregnancy.
The primary causes leading to maternal deaths include postpartum hemorrhage, hypertensive disorders during pregnancy, and infections. Sepsis, embolism, lack of access to healthcare facilities, and complications from unsafe abortions also contribute to the maternal mortality rates.
Where are the gaps that are increasing maternal mortality rates?
Timely and high-quality emergency obstetric care makes a huge difference between life and death for a woman during pregnancy and childbirth. Yet, there are several reasons why women are unable to receive life-saving treatment.
Delays, limitations, and inequitable access to obstetric care: timely access to emergency obstetric and newborn care can reduce maternal deaths by 15-50%. Currently, millions of women live beyond the safe travel time to healthcare centers, which can give them safe delivery options, conduct cesarean sections, provide blood transfusions, and provide life-saving medication. The limitations also affect newborn mortality rates.
Failures in quality of care, even for women who reach facilities: timely hypertension, hemorrhage prevention, prophylactic uterotonics, and sepsis protocols are the intricate steps that go into safe delivery. Close monitoring during labor hours can help prevent looming emergencies that may occur during delivery. While quality-collaborative improvement can narrow the disparities seen with severe maternal morbidity, scaling these efforts has been the main struggle.
Under-resourced information systems and feedback loops: while maternal and perinatal death surveillance systems are in place in many countries, reporting, compatibility, and research are often not up to par. Weak data quality impairs5 the real-time action and masks the preventable patterns.
Local and global crises are creating funding volatility: a recent example is the COVID-19 pandemic. Such local shocks can hinder and undo a lot of progress made in areas such as maternal health. Often, it can worsen current statistics, since healthcare resources6, such as services, staff, and supplies, are channeled away from maternal care. This can be catastrophic in fragile, conflict-affected areas.
Social and structural inequalities: social determinants would be one of the main factors impacting maternal mortality rates. Poverty, gender norms, intimate partner violence, socio-economic status, transport barriers, legal restrictions, and racism are just a few in the long list of structural hindrances. Even accessible clinical care cannot overcome these unless there is a policy change and enforcement of reform.
What is big data? How is big data contributing to women’s health?
Big data encompasses all the data extensively contributed from electronic health records, registries, lab systems, and datasets on various aspects of women’s health. The datasets require sophisticated methods, such as machine learning and language processing, to extract meaningful insights from all the data collected.
In breast cancer care7, AI algorithms are being applied to mammograms and pathology slides. This has helped reduce false positives and false negatives, enabling more accurate detection. Similarly, with health conditions such as PCOS, predictive models are being used to improve the diagnosis time, which can take an average of 2 years8. Integrating hormone data, ultrasound findings, and patient histories can offer a way to shorten diagnostic delays for a condition currently affecting 1 in 10 women globally.
Models for machine learning processes can be trained using pregnancy data to predict conditions like pre-eclampsia earlier9. This is often more accurate than traditional ways to do so. Early detection can favor timely interventions. Similar models are also being used to help clinicians identify women who are high-risk cases of postpartum hemorrhage10, enabling the preparation of blood products and uterotonics ahead of time.
Innovation is already helping close gaps in women’s health. But the key is scale and accessibility.
In what ways can big data help lower maternal mortality rates?
Big data can help systems run on autopilot, even during pandemics and other local strife, which can help prevent or escalate maternal deaths worldwide. Combining clinical records, geospatial mapping, and predictive analytics, a woman’s risk can be identified earlier, strengthening health system responses and holding providers accountable for negligence.
Risk prediction and early warning: as we have seen above, ML models can help predict complications such as preeclampsia, postpartum hemorrhage, and sepsis before they are life-threatening. For instance, algorithms trained with antenatal data, such as blood pressure, lab results, and demographics, can have higher chances of predicting preeclampsia when compared to traditional risk scores. These models can be integrated into electronic health records, especially among larger populations, to allow for predictions to be automatically triggered, flagging cases for referrals to higher-level facilities when required.
Continuity of care: predictive big data models can also identify women who are likely to be lost on follow-up. Based on various factors such as finances, transportation, and attendance of other appointments, resources can be allocated to enable continuity of care. Community health workers can regularly follow up, providing assurance, which is often a crucial step missing in the process. Linking all crucial data, both antenatal and postpartum, can help with smooth transfer across facilities if required.
Improving healthcare access through geospatial analytics: predicting emergencies is one of the most important factors contributing to maternal mortality risk. Geospatial modeling combined with big data can map travel times to healthcare facilities, where women can receive lifesaving services such as cesarean sections and blood transfusions. Several studies have shown that women across the globe live two or more hours from such care. Targeted investments into transport, maternity waiting homes, and upgrading local facilities are simple ways to reduce maternal deaths.
Standardizing emergency care: for women living far away, datasets can enable hospitals to build early warning dashboards that monitor blood loss, vital signs, and medications in real time at auxiliary health centers. Care can be delivered in real time based on progress during pregnancy or labor to prevent severe outcomes. Predictive models can also forecast blood product, care supplies, and other life-saving equipment requirements across facilities, preventing last-minute scrambling in emergencies. Pilot studies in the U.S. have shown that data-driven bundles reduce morbidity from hemorrhage. Similar approaches can be explored globally.
Maternal death surveillance: inconsistent reporting on pre- and postnatal data is one of the main struggles most regions encounter. Big data can digitize case reviews, code cases with standardized taxonomies, and automatically synthesize recommendations for health teams to analyze. Public and digital dashboards can track if corrective actions were taken and completed to provide an added layer of accountability. This ensures that no one is left behind. Regular surveillance and system upgrades ensure that women just don’t remain a statistic on the dashboard.
Tackling inequalities through linked data: a stark disproportionality is noticed in maternal deaths among poor, rural, and marginalized women. Linking health data with information relating to poverty, accessibility, and regional conflict allows governments to prioritize interventions for vulnerable groups. Solutions big data can provide are by integrating facility data with poverty maps, which can help identify regions where maternal mortality is concentrated. This can help, in some ways, eliminate the social barriers hindering medical care.
The bottom line
While big data on its own is not going to solve the maternal mortality crisis, it can help in significant ways to lower the numbers. Big data predicts risk, ensures continuity of care, optimizes access, and standardizes the emergency response. The key for the future is the operational will to make the change for women's health, placing equity and sustainability at the forefront.
References
1 UNICEF Data. (2025, April). Maternal mortality rates and statistics.
2 UNICEF Data. (2025, April). Trends in maternal mortality 2000 to 2023.
3 Moyer, C. A. (2023, February 23). Stalled progress in reducing maternal mortality globally. The Lancet.
4 Souza, J. P., Tunçalp, Ö., Vogel, J. P., Bohren, M., Widmer, M., Oladapo, O. T., et al. (2023, December 6). A global analysis of the determinants of maternal health and transitions in maternal mortality. The Lancet Global Health.
5 Birabwa, C., Banke-Thomas, A., Semaan, A., van Olmen, J., Kananura, R. M., Arinaitwe, E. S., Waiswa, P., & Beňová, L. (2024). The quality of routine data for measuring facility-based maternal mortality in public and private health facilities in Kampala City, Uganda. Population Health Metrics, 22(22).
6 Reuters. (2025, April 6). Aid cuts could leave more women dying in pregnancy and birth, UN says.
7 McKinney, S. M., Sieniek, M., Godbole, V., Godwin, J., Antropova, N., Ashrafian, H., Back, T., Chesus, M., Corrado, G. S., Darzi, A., Etemadi, M., Garcia-Vicente, F., Gilbert, F. J., Halling-Brown, M., Hassabis, D., Jansen, S., Karthikesalingam, A., Kelly, C. J., King, D., Ledsam, J. R., … Shetty, S. (2020, January 1). International evaluation of an AI system for breast cancer screening. Nature, 577(7788), 89–94.
8 Gibson-Helm, M., Teede, H., Dunaif, A., & Dokras, A. (2017). Delayed diagnosis and a lack of information associated with dissatisfaction in women with polycystic ovary syndrome. The Journal of Clinical Endocrinology & Metabolism, 102(2), 604–612.
9 Ranjbar, A., Montazeri, F., Rezaei Ghamsari, S., Mehrnoush, V., Roozbeh, N., & Darsareh, F. (2024). Machine learning models for predicting preeclampsia: A systematic review. BMC Pregnancy and Childbirth, 24, Article 6.
10 Venkatesh, K. K., Strauss, R. A., Grotegut, C. A., Heine, R. P., Chescheir, N. C., Stringer, J. S. A., Stamilio, D. M., Menard, K. M., & Jelovsek, J. E. (2020). Machine learning and statistical models to predict postpartum hemorrhage. Obstetrics & Gynecology, 135(4), 935–944.