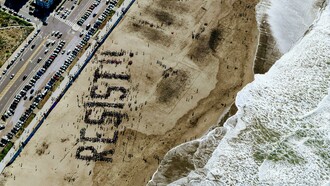We sat in a hospital conference room, my mother, siblings and I, together with our family physician. The issue at hand was my father’s deteriorating health, for which we had been summoned from across the country. In medical detail he described multiple system failures happening inside my father’s 73-year-old body, with the presumed eventuality of his death in the very near future.
With the ripple of this unwelcome news still echoing in my thoughts, I asked our doctor, who was also on the state board of medical ethics, if he had conveyed this diagnosis to my father.
“I have never been able to speak about an upcoming death with any patient- it has always been too difficult for me. This must be because it brings up my own fear of death and dying”. As he spoke, I was surprised by the tears in his eyes.
“He is your patient, but he is also your friend,” I said. “Could you speak to him? What you just told us, as his friend?” He nodded and said he would, and left the room.
As it turned out, my father survived his brief time in the ICU and was transferred to a nursing home for follow-up care. Some weeks later his breathing became too difficult and he died of chronic obstructive pulmonary disease (COPD).
Along with experiencing the loss of a parent, the memory of the conversation with our family physician persisted over the years. The realization dawned that what we just witnessed was not unusual and rare, but on the contrary. Our family physician had articulated an underlying fear which resided in many medical professionals throughout America and the world. A foreboding which contributed, most likely, to extended, sometimes painful and often heroic treatments for those approaching their natural time of leaving this world.
What if this fear could be diminished? How might that change the interactions between physicians and their patients, and the quality of being at the end of life?
A growing sense continued in me that this issue was in fact connected to another reality facing the healthcare community. How are physicians, nurses, chaplains, therapists- those professionals encountering the process of dying on a daily basis, not just in the experience of a parent or close relative passing- how are they coping? How are they dealing with the feelings and grief of constant, repeated exposure to another person’s death?
Ten years later, in response to these questions, a recording project was born. As a result of the phenomenal efficacy of Graceful Passages, in which music with spoken word was used to address the subject of dying for all of us, these questions concerning those in healthcare were addressed with a similar artistic approach.
A question was asked of leading physician educators and other health professionals across America, and their response was recorded:
If you were able to speak to your peers- to other health professionals- to possibly reduce their stress, their anxiety- what have you found helpful to carry through challenging times?
Joined by film composer Gary Malkin and a team of volunteers and advocates for those in healthcare, the Care for the Journey project was undertaken. After recorded interviews were gathered, each message was accompanied by a customized music score, similar to the use of music in films.
A nonprofit named Companion Arts was formed to support its mission, which included both educational programs for healthcare professionals and recordings.
Speakers were chosen from various aspects of healthcare, among them Ira Byock, MD, author and leader in palliative care; Angeles Arrien, PhD, anthropologist with a view to healthcare from a cross-cultural global perspective; Rachel Naomi Remen, MD, author and educator; Naomi Judd, RN, award-winning singer; Archbishop Desmond Tutu, advocate and activist; Jean Watson, RN, PhD, nurse leader and founder of Caritas; Joan Borysenko, PhD, author and pioneer of integrative medicine, and others.
Jeremy Geffen, MD, oncologist and author, spoke to the issue of balancing control and letting go.
What is the heart of healing?
The heart of healing is found in focused action and intention wrapped in the arms of surrender. Focused action and intention wrapped gently in the arms of surrender. Not only for patients and their loved ones, but also those of us who’ve devoted our lives to the service of healing.
To remember, even in our work of service, at the end of the day, we are really not in control. All we can do is bring our love, our presence, our consciousness, our intent to be present with what is happening, to smile with love if we can, to take action whenever we can, and to try always, to have our actions, and our intention, and our efforts, wrapped in the arms of surrender and gratitude.
Christina Puchalski, MD, founder of the George Washington Institute for Spirituality and Health, shared these words:
Whatever is your role, if your patient feels connected to you, if it comes from a place of intimacy, he’s much more likely to trust, much more likely to share.
And if he shares a joke or a story, laugh with him. Don’t be afraid to be yourself, don’t hide behind whatever clinical role you think you have. If he cries, let him cry and sit in silence with him, holding his tears for him in the midst of that pain. Be open. Just be with him. Let your conversations flow between obtaining the information that you need. But equally important, let the emotions also have their place.
And you in turn are much more likely to be able to heal, to be able to care, to be able to make a difference.
The Care for the Journey project resulted in two published CDs; the first volume released in 2005, the second in 2010. Thousands of these were distributed as gifts to nurses and other health professionals in hospital systems across America. Responses poured in from administrators, health professionals, educators, and patients, testifying to the sincerity of the messages and the undying power of combining words with music.
The original questions which birthed this project remain woven into the existential fabric of our contemporary society. In the thirty years since we met with our family physician, so much has changed in the attitude which health professionals hold about death.
Still, for many, the belief that death represents a medical defeat remains embedded. It is our hope that, as recognition grows of our essential relationship to the dying process, humans- and especially those entrusted with their care- become less governed by a fear of death and more open to the natural rhythms of life.