This is the second of a series of articles that I am writing about tests, vaccines and treatments for COVID-19. The goals are to describe diagnostic and antibody tests as well as progress being made in developing vaccines and treatments.
Diagnostic tests for viral antigens (active infection by the SARS-CoV-2 virus)
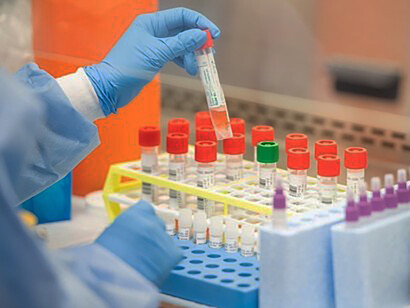
Diagnostic tests look for the presence of viral antigens in the blood and/or saliva. When present, these antigens indicate that the person has an active infection1. That is, the SARS-CoV-2 virus has proteins on its surface which act as antigens. They stimulate the immune system to produce antibodies, which indicate previous exposure to the virus. Antibodies bind to viral antigens, triggering an efficient immune response in most people. So, the presence of antigens indicates an active infection, while antibodies indicate that the person being tested had previous exposure to the virus. This section will focus on diagnostic tests, which look for the spike (S), nucleocapsid (N) and/or envelope (E) proteins1.
The citizens of Wuhan are heroes. Their cooperation during nearly 11 weeks of lockdown helped save countless lives by containing the spread of the SARS-CoV-2 virus and the COVID-19 disease. Confining 11 million people seemed to be nearly impossible. On March 24, after no new local infections were recorded for several consecutive days, officials announced plans to end the mass quarantine. After being reopened, Chinese labs tested 9.9 million people in an unprecedented 19-day campaign from May 14 to June 1. They found only 300 people who were infected. None of them had symptoms. Then, close contacts of those infected were tested. No infections were found in the 1174 close contacts. This was done at no cost to the individuals. In contrast, when some people in the USA wanted a diagnostic test, they were told to wait until they have trouble breathing. Then, they went to the nearest hospital (which might be hundreds of km away) to be tested. Some had to pay for an ambulance, time in intensive care, and time in the hospital. This can amount to as much as $10,000 – a cost that can drive many people into bankruptcy – especially if they lost their job. In China and other countries with health care for all, the test is free - as is the stay in the hospital. It the USA, the test can cost a person almost everything that they have if they don’t have adequate health insurance.
As described last month1, most currently used tests for the virus use a reverse transcriptase polymerase chain reaction (RT-PCR). These tests look for viral RNA in samples taken from a nasopharyngeal swab. A new test developed in the Rutgers Clinical Genomics Lab can analyze saliva or viral RNA2. In contrast, Iceni Diagnostics’ at-home test kit recognizes specific carbohydrates (glycans) that are part of the viral glycoproteins3. A duplex Coronavirus/generic flu test is also being developed to identify both viruses in one sample1,3.
In the meantime, Sherlock Biosciences is also developing a diagnostic test that can be done at home4. It’s based on an Internal Splint-Pairing Expression Cassette Translation Reaction (INSPECTR). “It is a synthetic biology-based platform designed to enable the creation of an instrument-free, handheld diagnostic test—similar to an at-home pregnancy test—that can be applied across multiple diseases and in numerous settings”. It uses CRISPR technology to detect almost any DNA or RNA sequence in any pathogen4.
Tests for antibodies (previous exposure to SARS-CoV-2)
The US FDA and regulatory agencies of other governments have approved the use of antibody tests that can detect past infections after people have recovered and even if they had no symptoms of COVID-19. The tests analyze blood samples in authorized laboratories. The first three tests approved by the FDA look for IgM antibodies, which are present earlier in infection. In comparison, Abbott Laboratories has an antibody test that looks for IgG antibodies, which are produced later. Abbott's IgG antibody test will be able to perform up to 100-200 tests per hour. Even if a person has IgG and/or IgM antibodies, we don’t know how long the immunity will last.
The FDA published the first validation results of 12 COVID-19 antibody tests5. These tests must be very accurate. If only about 5% of the population is been infected with the SARS-CoV-2 virus, then just flipping a coin will be accurate 95% of the time. So, it’s good that Abbott Lab’s test for IgG antibodies had a sensitivity of 100%, a specificity of 99.6%, and positive and negative predictive values of 92.9% and 100%, respectively. Also, a two-step ELISA test developed by clinical laboratories at the Mount Sinai Health System in New York had a sensitivity and specificity of 92.5% and 100%, resulting in positive and negative predictive values of 100% and 99.6%. The results for all 12 FDA approved tests were given5.
Treatments for COVID-19
The malaria drug hydroxychloroquine that was touted by some politicians is no longer approved by the FDA or the WHO. On the other hand, the antiviral prescription drug remdesivir lowered the recovery time of patients who had COVID-19 to 11 days, compared to 15 days for patients who received placebo6. The FDA issued an emergency use authorization for it. However, it does not help patients once they become critically ill. Fortunately, an inexpensive and relatively safe steroid called dexamethasone was shown to decrease the mortality (save lives) of patients who had COVID-19 and were on ventilators or are on oxygen7. A total of 2104 patients received 6 mg of dexamethasone once per day (either by mouth or by intravenous injection) for ten days. They were compared with 4321 patients who received usual care only (control group). In this control group, the 28-day mortality was highest in those who required ventilation (41%), intermediate in those patients who required oxygen only (25%), and lowest among those who did not require any respiratory intervention (13%). In comparison, dexamethasone reduced deaths by one-third in ventilated patients (rate ratio 0.65) and by one fifth in other patients receiving oxygen only (rate ratio 0.80). There was no benefit for those patients who did not require respiratory support7.
In addition, some success has been made by using antibodies from volunteers who have already been exposed to the virus. They are donating blood plasma, which contains thousands of different antibodies that bind to viral antigens, triggering an immune response. However, not all antibodies are the same. Some are much more active than others. So, donors who have more active antibodies are especially useful in curing patients with active infection and severe symptoms. Moreover, labs are isolating the best antibodies and cloning them to make monoclonal antibodies. Eli Lilly and Company has started the first human trial of an antibody therapy called LY-CoV555. The treatment was created in collaboration with AbCellera, a Canadian biotechnology company. Scientists at AbCellera and the United States Vaccine Research Center at the National Institute of Allergy and Infectious Diseases selected the most potent antibodies. Eli Lilly scientists engineered monoclonal antibody therapy. This approach has worked to treat other diseases, including HIV, asthma, lupus, Ebola, and some forms of cancer. A monoclonal antibody might also be useful as prevention for vulnerable patient populations for whom vaccines might not be a good option. Examples include the elderly or people who have chronic diseases or compromised immune systems. Eli Lilly has already begun manufacturing the monoclonal antibody LY-CoV555 in large quantities so it can be tested in Phase 2 trials.
Regeneron has started a clinical trial of a mixture of two antibodies (REGN10933 and REGN10987) that bind non-competitively to the receptor binding domain of the viral S protein8. This is similar to an Ebola treatment (REGN-EB3) that they developed and tested in a clinical trial conducted in the Congo. The trial for REGN-COV2 will consist of four separate study populations: Hospitalized COVID-19 patients; non-hospitalized symptomatic COVID-19 patients; uninfected people in groups that are at high risk of exposure, such as healthcare workers or first responders; and uninfected people with close exposure to a COVID-19 patient, such as the patient’s housemate. If successful, the treatment might be available by the fall8.
Vaccine development
Vaccine candidates are being developed, while others are already in clinical trials. Genetic Engineering & Biotechnology News has a website that tracks news, milestones, and updates on more than 200 drug and vaccine candidates currently being developed for the COVID-19 pandemic9,10. Three vaccine candidates have passed Phase 1 and are entering Phase 2 clinical trials. They are all using a genetically engineered cold virus (Adenovirus Type 5) as the vector or vehicle that delivers the viral gene that codes for the spike (S) protein. One advantage is that adjuvants are not needed. These are immunological or pharmacological substances that improve the immune response of a vaccine. Alum, analgesics, paraffin oil, bacterial products, squalene, saponins, cytokines and Freund’s complete adjuvant have been used as adjuvants in previous vaccines. The adenoviruses themselves drive the inflammation, which is kept under control by giving the vaccines at low doses. Traditional vaccines, made from weakened viruses or viral proteins, stimulate B cells to make antibodies against the virus. Those antibodies bind to specific proteins on viruses and prevent them from entering our cells. The problem is that once the virus infiltrates our cells, the antibodies from a traditional vaccine are useless. It’s at that stage that T cells are needed. Adenovirus vectors are pre-eminent in inducing a strong T-cell response. However, no adenoviral vector vaccines have been able to prevent any diseases in humans so far9,10. The ChAdOx1-S vaccine that expresses the spike (S) glycoprotein in a recombinant adenovirus type-5 vector is in Phase 2b/3 trials. It was developed by the University of Oxford and AstraZeneca. It recently completed a successful Phase 1 trial on 108 healthy volunteers in Wuhan, China11. It was both safe and induced an immune response. Three different doses were tested – 6x1010, 1x1011 and 1.5x1011 viral particles. All three doses induced both specific antibody and T-cell responses. Antibodies targeting the S protein viral antigen increased after day 14 and peaked after 28 days11.
CanSino Biological Inc./Beijing Institute of Biotechnology are testing an Adenovirus Type 5 vector9. Moderna and NIAID developed a lipid nanoparticle (LNP) encapsulated mRNA.
Four other vaccines are in Phase 1/2 clinical trials. Three of them are based on inactive viruses. They were developed by Wuhan Institute of Biological Products/Sinopharm, Beijing Institute of Biological Products/Sinopharm, and Sinovac. The fourth vaccine candidate in Phase 1/2 clinical trials is a vaccine developed by Novavax. It is based on a recombinant SARS-CoV glycoprotein nanoparticle with a Matrix M adjuvant. BioNTech, Fosun Pharma and Pfizer developed a vaccine containing three LNP-mRNAs. One other vaccine has started a Phase 1 clinical trial. There are also 123 candidate vaccines in preclinical evaluation. This is a cooperative effort. The U.S. National Institute of Health (NIH), the European Medicines Agency, and more than a dozen biopharmaceutical companies are prioritizing and accelerating clinical study of drug and vaccine candidates9.
In Phase 1 (also called Phase I) trials, small groups of people receive the trial vaccine12. In Phase 2, the clinical study is expanded. The vaccine is given to people who have characteristics (such as age and physical health) similar to those for whom the new vaccine is intended. In Phase 3, the vaccine is given to thousands of people and tested for efficacy and safety. The goals of Phase 1 testing are to assess the safety of the candidate vaccine and to determine the type and extent of the immune response that the vaccine provokes. Phase 2 trials use more participants. Some may belong to groups at risk of acquiring the disease. These trials are randomized and well-controlled and include a placebo group. The goals of Phase 2 testing are to study the candidate vaccine’s safety, immunogenicity, proposed doses, schedule of immunizations, and method of delivery. Successful Phase 2 candidate vaccines continue to larger Phase 3 trials, involving thousands to tens of thousands of people. These Phase 3 tests are randomized and double-blind. The experimental vaccine is tested against a placebo. The placebo may be a saline solution, a vaccine for another disease, or some other substance. After licensure, the FDA will continue to monitor the production of the vaccine. Production facilities will be inspected regularly. The FDA and other countries’ regulatory agencies will review the manufacturer’s tests of all lots of vaccines for potency, safety and purity. A Phase 1/2 trial tests the safety, side effects, and best dose of a new treatment or vaccine. In the phase 2 part of the clinical trial, patients usually receive the highest dose of vaccine that did not cause harmful side effects in Phase 1. Combining phases 1 and 2 may allow research questions to be answered more quickly or with fewer patients12.
Fortunately, it appears that recovered patients retain their immunity and have a robust response13. A recent study documented a robust antiviral immune response to SARS-CoV-2 in a group of 20 adults who had recovered from COVID-19. The findings show that the body’s immune system is able to recognize SARS-CoV-2 in many ways, dispelling fears that the virus may elude ongoing efforts to create an effective vaccine13.
It’s also important to protect our young children. In the USA, only about 1.7% of all the people who have tested positive for the SARS-CoV virus are children younger than 18 years (1.1% in the Netherlands, and 2.0% in the UK) 14. A survey conducted by the United States Centers for Disease Control and Prevention, children aged 17 and under, who make up 22% of the US population, account for fewer than 2% of confirmed COVID-19 infections across the United States. There were 2572 children in the survey. Only 5.7% went to the hospital and only three died. Children seem to have a stronger and more effective initial immune response to the virus than adults. They might have some immunity from recent exposure to similar viruses. More importantly, children have much stronger blood vessels. It’s primarily adults who form clots in their blood vessels. In some patients, this leads to heart attacks or strokes. Normally, blood clots form only to stop bleeding from an injury, but if the endothelium is damaged, clots can also form. The SARS-CoV-2 virus can infect endothelial cells, which exist throughout the body15.
Unfortunately, there is a possibility that a small proportion of young children who become infected with the virus can develop a severe heart disease similar to Kawasaki disease that can lead to cardiac aneurysms14. There appeared to be a small outbreak in the city of Bergamo, Italy during the height of the outbreak of COVID-19 in that country. There was a report of ten cases of children developing Kawasaki-like disease. At this time, we don’t know if the SARS-CoV-2 virus triggered the disease or is simply a new disease that has emerged with unknown causes. For now, the disease is called pediatric inflammatory multisystem syndrome temporarily associated with SARS-CoV-2 (PIMS-TS). It is possible that it is mediated by antibodies or immune complexes since there was little evidence that the virus was replicating in these children. “If this is an antibody-mediated phenomenon, there might be implications for vaccine studies, and this might also explain why some children become very ill with COVID-19, while the majority are unaffected or asymptomatic” 14.
As mentioned last month, a mutant form of the SARS-CoV-2 virus has emerged and become dominant1. Amino acid 614 in the mutant is a glycine (G), but D-aspartate (D) in the original virus. This is called a D614G mutation1. In a study this month, it was shown that this mutation in the S protein made it more stable and the virus more infective. The density of S proteins on the surface of the virus increased four to five times over the original form. As a result, each mutant virion particle can infect human hose cells more efficiently. This could help explain why the SARS-CoV-2 virus has spread so rapidly throughout most of the Americas. The G614 genotype was not detected in February (among 33 sequences) and existed at low frequency in March (26%), but increased rapidly by April (65%) and May (70%), indicating a transmission advantage over viruses with D61416. Others have estimated that it was almost 100% prevalent by the end of April17. Fortunately, both genotypes (D614 and G614) are similarly susceptible to neutralizing antisera, indicating that antibody-mediated control of viruses carrying SD614 and SG614 would be similar.
Glossary of Terms
Antibodies. Proteins made by immune cells that bind to antigens from a pathogen (like the spike protein in the SARS-CoV-2 virus).
Antigens. Parts of a pathogen (like the spike protein in the SARS-CoV-2 virus) that induces the production of antibodies in a host cell.
CDC. Centers for Disease Control (in the USA).
Cytokines. Chemical signaling molecules that guide a healthy immune response.
IgG (Immunoglobulin G) antibody: Antibodies released by B cells that bind to pathogens and activate the classical pathway of the complement system. These are the most abundant antibodies in human blood serum.
IgM (Immunoglobulin M) antibody. Antibodies that block the binding of pathogens to host cells and by aggregating infectious agents to facilitate their clearance.
Monoclonal antibody. An antibody made from a single clone or cell line and consisting of identical antibodies.
Polymerase Chain Reaction (PCR). A way to amplify (make many copies) of DNA, using a reaction catalyzed by a DNA polymerase.
Reverse transcription. Transcription of RNA into DNA.
Reverse transcriptase polymerase chain reaction (RT-PCR). A way to test for RNA. It combines reverse transcription of RNA into complementary DNA (cDNA), followed by amplification of specific DNA targets.
Notes
1 Smith, R.E. Developing Vaccines and Treatments for COVID-19. Humans Are Not the Enemy. Wall Street International, May 24, 2020.
2 US FDA. Accelerated Emergency Use Authorization (EUA) Summary SARS-CoV-2 Assay.
3 Katori, S. Iceni Diagnostics Eyes Fall Release of At-Home Coronavirus Test. ClinicalOmics, 6 May, 2020.
4 Sherlock Accelerates COVID-19 Dx Development, Launches Innovation Lab. Clinical Omics, 21 May, 2020.
5 FDA. EUA Authorized Serology Test Performance. 15 June, 2020.
6 Ledford, H. Hopes rise on Coronavirus drug remdesivir. Nature, 29 April, 2020.
7 University of Oxford. Dexamethasone reduces death in hospitalised patients with severe respiratory complications of COVID-19. 16 June, 2020.
8 Philippides, A. Regeneron launches trials of COVID-19 antibody cocktail. Genetic Engineering & Biotechnology News, 11 June, 2020.
9 Cross, R. Adenoviral vectors are the new COVID-19 vaccine front-runners. Can they overcome their checkered past? Chemistry & Engineering News, Volume 98, issue 19, 12 May, 2020.
10 WHO. Draft landscape of COVID-19 candidate vaccines, 2 June 2020.
11 Zhu F-C et al. Safety, tolerability, and immunogenicity of a recombinant adenovirus type-5 vectored COVID-19 vaccine: a dose-escalation, open-label, non-randomised, first-in-human trial. The Lancet, published online 22 May, 2020.
12 CDC. Vaccine Testing and the Approval Process, 2020.
13 Recovered Patients Show Robust Immune Response to SARS-CoV-2. Clinical Omics, 18 May, 2020.
14 Viner, R.M. and Whittaker, E. Kawasaki-like disease: emerging complication during the COVID-19 pandemic. The Lancet, Volume 395, pp. 1741-1743, 2020.
15 Varga, Z. et al. Endothelial cell infection and endotheliitis in COVID-19. The Lancet, Volume 395, pages 1417-1418, 2020.
16 Zhang, L. et al. The D614G Mutation in the SARS-CoV-2 Spike Protein Reduces S1 Shedding and Increases Infectivity. Scripps Research, 2020.
17 Cortey, M. et al. SARS-CoV-2 Amino Acid Substitutions Widely Spread in the Human Population Are Mainly Located in Highly Conserved Segments of the Structural Proteins. BioRxiv preprint, 17 May, 2020.