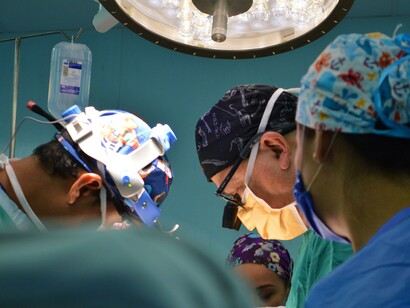
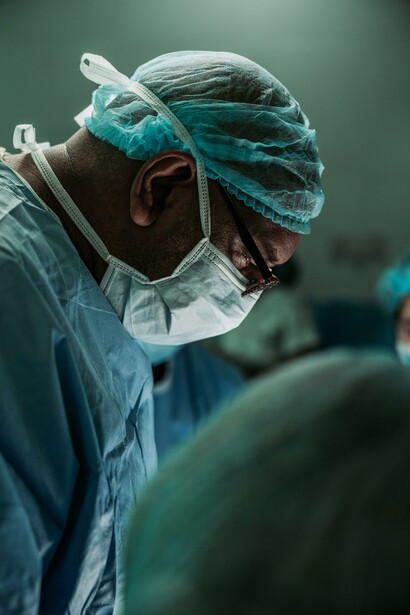
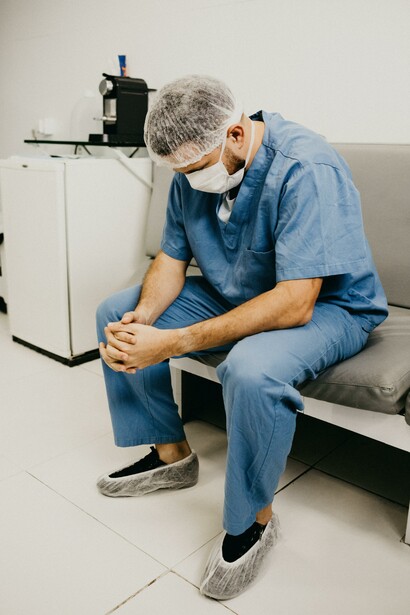
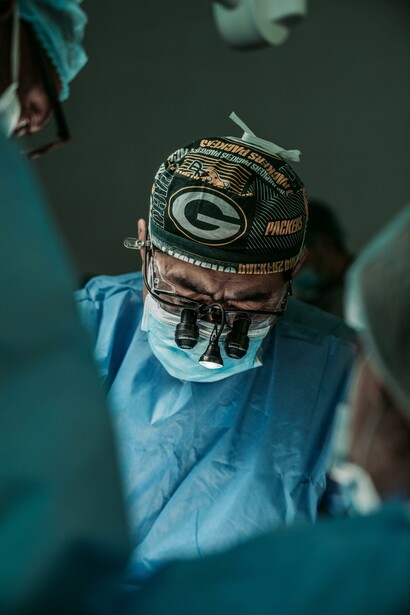
During my summer studying in Greece, I had the opportunity to interview Jeffrey Levett, the director of Greece’s Department of Health Management and the founding dean of the National School of Public Health in Athens. When I asked him: “What is successful about Greek healthcare?” his answer was surprising. He told me, among other things, that the dedication of Greek nurses and doctors to provide the people with adequate healthcare was truly impressive, especially considering how many budgetary and other bureaucratic restrictions they constantly face. His sentiment seemed to be repeated when we talked to Balasopoulos Anastasia, the director of Hippocratio, a large teaching hospital in Athens. She told us that, out of all the staff working in the hospital, she respected the doctors and nurses “working on the front lines” the most.
The admiration that all these major public health figures had for their doctors was really refreshing compared to the way that doctors seem to be demonized by people not directly involved with healthcare. I have heard many people, from both Greece and America, claim that their doctors aren’t spending enough time with them, aren’t listening to their problems, and are making too much money. After a year and a half, though, of working in, observing, and learning about healthcare systems, I have realized that doctors deserve a lot more sympathy than they get. Becoming a doctor, especially in America, is a long, difficult process, and even when people do finally become board certified, they often face many mental and physical health difficulties because of their occupation. On trend, physicians everywhere are losing their motivation, their love and compassion for others, and their commitment to provide only the best healthcare possible, and that fact puts each one of their patients at risk.
While we were touring Hippocratio, one of the cardiologists offered our group a morsel of guidance: “Doctors are not scientists. They are hard workers. If you guys really do want to become doctors, you must be ready to work hard.” Almost every single doctor I have met in the past five years has warned me about how difficult it is to be a doctor. Being successful in any career requires hard work and dedication, so why are doctors so certain that their careers are more arduous than other careers? They make tons of money, so their lives can’t be that bad, right?
Well, according to a study done by Medscape in 2019, anywhere between 32-48% of doctors are burned out. Medscape asked the doctors they surveyed what contributed most to their burnout, and many of the doctors mentioned bureaucratic tasks (59%), spending too many hours at work (34%), and lack of respect from administrators, colleagues, and staff (30%) as being the biggest causes. The same article found that, in about 53% of the doctors that faced burnout and depression, their mental frustrations interfered with their work and caused them to be more easily exasperated with patients, feel less motivation, and occasionally make mistakes they wouldn’t normally make. To me, though, the most startling figure comes from an article by Scientific American: The suicide rate for doctors is twice as high as it is for the general population.
In fact, there isn’t any real debate that doctors are chronically depressed; a quick Google search of “why are doctors so unhappy” results in a plethora of major research groups coming to the same conclusions: The work of doctors is frustrating, patient care is suffering from it, and the cause of this physician burnout is extremely complicated and probably due to problems that extend from the roots of entire healthcare systems. Frankly, the complexity of this issue is daunting, especially to a second-year premedical student. But, if there is something in all this worth focusing on, it is the question "how do we solve the physician burnout crisis and make medical work more fulfilling?”
Some articles, like one published in MD Magazine, suggest that doctors make lifestyle changes (like meditation, exercise, and better scheduling) that decrease their stress levels and allow them to better handle the troubles of being a doctor. Frankly, I don’t think we should be blaming doctors for their own unhappiness. Doctors, just from the nature of how difficult it is to graduate medical school and complete their residencies, have extremely high levels of self-control and maturity; if they needed to make lifestyle changes in order to be happy, they are smart enough to have already made those lifestyle changes. This suggests that the problems with medical professions are more complex and systematic and that solutions like the ones proposed by MD Magazine, while helpful on an individual level, still only tackle symptoms of the major problem that doctors are facing: That the field of healthcare is rapidly changing with technology, that doctors are constantly being expected to do more than they are capable of, and that the entire career path of doctors needs to be overhauled so that doctors can have more career flexibility and the ability to take up managerial roles within their work environments.
The Hippocratic Oath is a double-edged sword for physicians. Doctors, in swearing to “do no harm” to their patients and hold their needs above their own, almost guarantee that they will be putting themselves under serious mental strain and risk even their physical health for the sake of other people’s wellbeing. However, the field of medicine demands this sort of mentality from its workers – Pamela Wible, MD, told Medscape, “Medical training teaches us to ‘suck it up’” and that “Because the majority of doctors are overworked, exhausted, and discontent, they’ve normalized their misery and pretend that it’s not as bad as it seems.”
Nothing makes me sadder than a clearly unhealthy and unhappy physician, yet, more and more, this seems to be the growing norm within medicine. Of course, healthcare should be focused on serving patients, but it shouldn’t also jeopardize the health of its workers. It is overwhelmingly clear to me that there needs to be changes to this field, big overhauls that encourage physician growth and development rather than their stagnation and eventual degradation post-residency. A big step towards this is for people to start having more empathy for their doctors and the stressful conditions, bull-crap bureaucracy, and horrible hours that they deal with every day. Physicians are human beings, too.
Bibliography
Farmer, B., & Kaiser Health News. (2018, August 6). Doctors Grapple with High Suicide Rates in Their Ranks. Retrieved June 10, 2019, from Scientific American.
Goodman, J. C. (2014, September 11). Why Are Doctors So Unhappy?. Retrieved from Forbes.
Kane MA, L. (2019, January 16). Medscape National Physician Burnout, Depression & Suicide Report 2019. Retrieved June 10, 2019, from Medscape.
Kelly, G. (2015, March 31). America’s Doctors: The Unhappy Richest 1%. Retrieved June 10, 2019, from MD Magazine.
Koenig MD, K. (2002, June 26). Why Are Doctors So Unhappy?. Retrieved June 10, 2019, from NEJM Journal Watch.
Kumar S. (2016). [Burnout and Doctors: Prevalence, Prevention and Intervention] (doi:10.3390/healthcare4030037). Healthcare (Basel, Switzerland), 4(3), 37.
West P. A. (2001). Why are doctors so unhappy? Calibre of people recruited to medicine may be too high for the job. BMJ (Clinical research ed.), 322(7298), 1361. Retrieved from NCBI.